Root Canal Treatment
Root Canal Treatment
Root canal therapy, also known as endodontic therapy, is a dental treatment for removing infection from inside a tooth. It can also protect the tooth from future infections. Root canal treatment has a false reputation for being very painful.
A tooth consists of a crown and roots. The crown is mainly above the gum, while the roots are below it. The roots attach the tooth to the jawbone.
Inside the crown and the root, or the root canal, is the pulp. The pulp nourishes the tooth and provides moisture to the surrounding material. The nerves in the pulp sense hot and cold temperatures as pain.Root canal treatment is carried out in the pulp of the tooth, which is the root canal.
Why do I need a root canal treatment?
Root canal treats infected or injured pulp. This helps to repair a tooth before it requires extraction.
If the pulp becomes injured or diseased, it cannot repair itself, and the tissue dies.If there is a deep cavity, a cracked tooth, or a loose filling, bacteria can enter the pulp. A pulp injury will make the tooth sensitive to high and low temperatures. There may be pain when chewing, and some people have a continuous, throbbing pain.
The bacteria will eventually destroy the pulp. If the bacteria penetrate through the root openings, it can cause an infection in the bone.
An infection will weaken the bone and break it down. The ligaments around the tooth will swell, and the tooth will become loose.
How is root canal treatment performed?
Root canal therapy is done in three steps, and it takes between one and three sessions to complete. The endodontist prepares for the procedure by examining and X-raying the tooth. Next, the dentist gives a local anesthetic to numb the tooth and places a protective covering (rubber dam) in the person’s mouth to isolate the damaged tooth and protect the rest of the mouth.
Cleaning the root canal
First, the dentist removes the decayed portion of the tooth and everything that is inside the root canal.A small access hole is made on the surface of the tooth and r the diseased and dead pulp tissue is removed with very small files.
Filling the root canal
Next, the dentist cleans, shapes and decontaminates the hollow area, using tiny files and irrigation solutions. Then, the tooth is filled with a rubber-like material, using an adhesive cement to seal the canals completely. Treatment often takes only one appointment, but if there are curved canals, multi-canals, or large infections, this could take one or two additional appointments.
After root canal therapy, the tooth is dead. The patient will no longer feel any pain in that tooth because the nerve tissue has been removed, and the infection has been eliminated. Any infection in the bone surrounding the tooth takes a couple of weeks to heal and show improvement on an intraoral xray.
Why is a cap needed for a root canal treated tooth?
The tooth will be now more fragile after a root canal treatment, than it was before. A tooth with no pulp must receive its nourishment from the ligament that attaches the tooth to the bone. This supply is adequate, but in time, the tooth will become more brittle, so a crown or filling offers protection.
Until the crown or filling is complete, the patient should not chew or bite on the tooth. Once there is a crown or filling is done, the person can use the tooth as before.
How painful is it to have a tooth treated ?
One of the great fears about this kind of treatment is that it will be painful, but the treatment that is carried out by a trained dental surgeon should be relatively painless.
The pain that is felt comes from the infection and not from the treatment. The treatment does not cause pain; it helps to alleviate it.
The dental surgeon will relieve the pain of the procedure by numbing the tooth and surrounding area with local anesthesia.
After the treatment, some tenderness is normal. It is temporary, and over-the-counter (OTC) pain medication may be enough to relieve it. If needed, he dentist may prescribe an antibiotic to treat or prevent infection.
Without treatment, the infection will spread. Eventually, the tooth will become loose and need extracting. Saving the natural tooth is best, if possible, because nothing functions as well as a natural tooth.
What if a tooth cannot be saved even with a root canal treatment?
Some patients opt for extraction, especially if it hurts a lot or if the tooth cannot be restored, for example, if there is large decay, trauma, or loss of bone due to periodontal, or gum, disease.
However, removing a tooth may mean that the surrounding teeth start to move and become crooked. This can look unsightly, and it can make it hard to have a good bite.
Are there any risks involved with root canal treatment?
As with any procedure, complications can occur.
- Sometimes the dentist only finds three root canals in a tooth that has four. If one canal remains untreated, the infection might continue and spread into the bone.
- The dentist must also make sure the filling material goes far enough into the canal, to fill it up. If the root canal is not properly sealed, the infection could return.
- During the procedure, the root of the tooth may crack, or the instruments can break in the canal or perforate the canal. This makes it hard to fill the tooth effectively.
If complications occur, a specialist can try to correct the problem and complete the root canal.
To avoid complications, patients should always follow the dentist’s instructions. If an antibiotic is needed, it is important to finish the entire prescription.
It is essential to have a permanent restoration placed, such as a crown, once the root canal therapy is complete.
How much pain is normal?
Most people report feeling a little sensitive or tender for a few days after having a root canal.
There are several reasons for this:
- The tissue around the gums remains swollen or inflamed: Even though the dentist has removed the nerve root from the tooth, there are still small nerves in the ligaments and tissue surrounding the tooth. When this area is inflamed, such as after a dental procedure, these nerve endings can also register discomfort.
- Instrument damage: It is possible that a dental instrument used to clean out the root canal inadvertently damaged the sensitive surrounding tissue.
- High temporary filling: This is when the dentist put in the temporary filling and they did not smooth it down enough. If the filling is even just a little higher than the surrounding tooth, it can cause the mouth to bite harder on that spot, which would make the tooth sore.
In most cases, the sensitivity and discomfort associated with a root canal should go away within a few days.
If it does not get better, or if the pain is severe or unrelieved by home measures, it is important to call the endodontist or dentist for an evaluation.
Can a root canal fail?
Fortunately, most root canals are successful. However, some root canal treatments are unsuccessful, and a person can experience more pain. There are many reasons why this happens:
- The restoration begins to leak
- Poor oral or dental hygiene
- Breakdown of the tooth or sealing material over time
- Presence of an extra canal in the tooth that the endodontist cannot see
- An obstruction such as a curved root canal that prevents complete cleaning of the canal
- Vertical cracks in the tooth
- Dentist or endodontist error
If the cause of the pain is due to a missed canal, the endodontist will need to open the tooth, remove the filling and try to find the canal.
If the tooth has a vertical fracture, the dentist would likely have to remove the tooth.
If a person experiences persistent inflammation or infection after a root canal, they may require a surgical procedure called a root-end resection.
When can treating a failed root canal be reattempted?
With proper care, even teeth that have had root canal treatment can last a lifetime. But sometimes, a tooth that has been treated doesn’t heal properly and can become painful or diseased months or even years after treatment. If your tooth failed to heal or develops new problems, you have a second chance. An additional procedure may be able to support healing and save your tooth.
As occasionally happens with any dental or medical procedure, a tooth may not heal as expected after initial treatment for a variety of reasons:
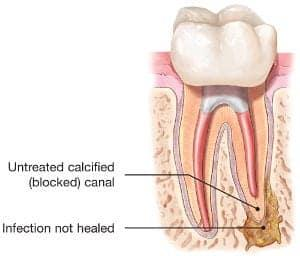
- Narrow or curved canals were not treated during the initial procedure.
- Complicated canal anatomy went undetected in the first procedure.
- The placement of the crown or other restoration was delayed following the endodontic treatment.
- The restoration did not prevent salivary contamination to the inside of the tooth.
In other cases, a new problem can jeopardize a tooth that was successfully treated. For example:
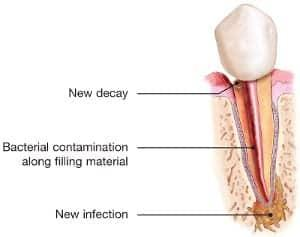
- New decay can expose the root canal filling material to bacteria, causing a new infection in the tooth.
- A loose, cracked or broken crown or filling can expose the tooth to new infection.
- A tooth sustains a fracture.
First, the endodontist will discuss your treatment options. If you and your endodontist choose retreatment, the endodontist will reopen your tooth to gain access to the root canal filling material. In many cases, complex restorative materials—crown, post and core material—must be disassembled and removed to permit access to the root canals.
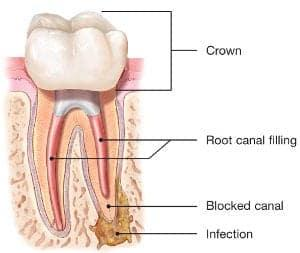
After removing the canal filling, the endodontist can clean the canals and carefully examine the inside of your tooth using magnification and illumination, searching for any additional canals or unusual anatomy that requires treatment.
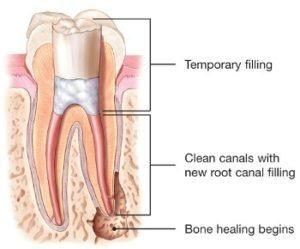
After cleaning the canals, the endodontist will fill and seal the canals and place a temporary filling in the tooth. If the canals are unusually narrow or blocked, your endodontist may recommend endodontic surgery. This surgery involves making an incision to allow the other end of the root to be sealed.
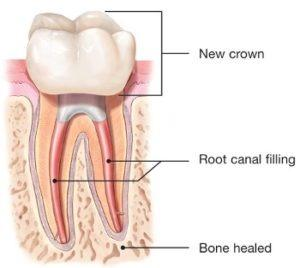
After your endodontist completes retreatment, you will need to return to your dentist as soon as possible to have a new crown or other restoration placed on the tooth to protect and restore it to its full function.
